Introduction
In March early on in this pandemic I first drew attention to some ultra-left errors on the COVID outbreak. [1] In that article I also outlined some of the salient science. In several articles since I have elaborated on these issues. However, a persistent ultra-leftist ‘denialist’ stance has continued to make itself heard. The remarkable coincidence of these views with some of the ultra-right wing is a sorry spectacle. [2]
I do not wish to re-tread old ground, but a series of misperceptions about the death rates in Sweden prompt this short review. Some have argued that Sweden, while not undergoing severe lock-down, has experienced good outcomes. Naturally no thinking Marxist can see the Swedish state as ever having been a bastion of socialism. However it has been a relatively liberal state.
As if to show that this was only a façade, the state adopted very anti-science based policies in handling its COVID epidemic. Led by a strong willed epidemiologist (Anders Tegnell) it adopted a policy for no or very minimal ‘lock-down’ and mask wearing, to build up a so-called ‘herd immunity’. This also supposedly would leave the economy unscathed. Such nonsense has been shown to be a complete failure on both counts:
“there’s so far limited evidence that Sweden’s decision to leave much of its society open will support the economy. Finance Minister Magdalena Andersson recently warned that Sweden is facing its worst economic crisis since World War II, with GDP set to slump 7% in 2020, roughly as much as the rest of the EU.” [3]
In the process it also unveiled a remarkably cynical view on the expendability of old people. There is no need to expend energy in polemicising on this. It is remarkable that any leftist might be taken in by the Swedish experience. We only try here to offer a view of the scientific literature at the moment on COVID-19 and death rates, in particular as related to Sweden.
1) Sweden knocked off the old with COVID
Simply put, the true mortality rates from Sweden cannot be reliably estimated in the old as there is significant pressure to under-report these figures. This can be seen from anecdotal reports, now widely circulating in the lay press, about how people in old age homes are ‘allowed to die’ without support. See for instance this vignette in the WSJ – which in this case has a happy ending:
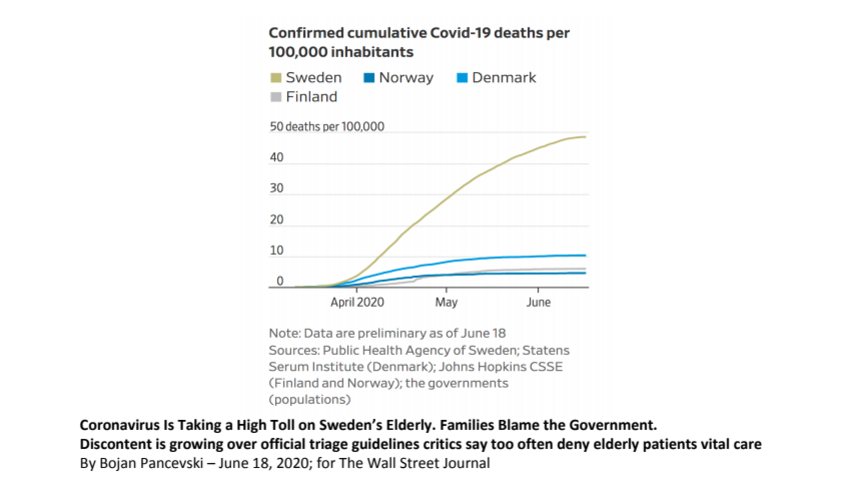
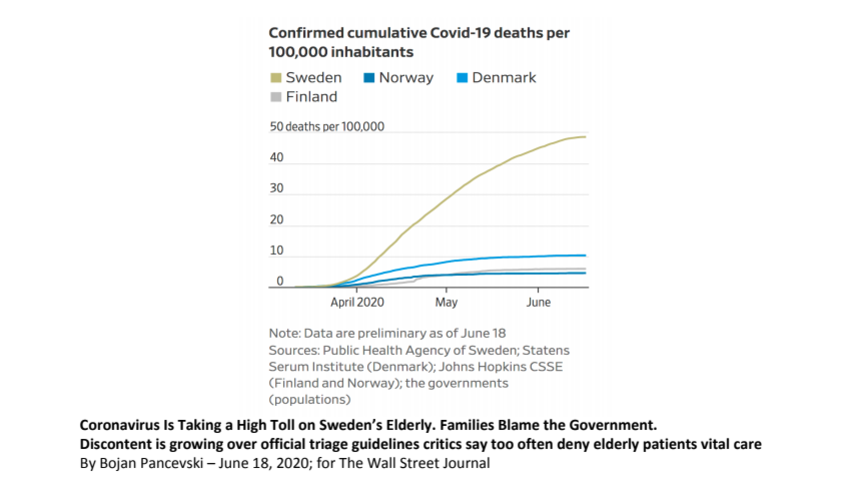
“When 81-year-old Jan Andersson fell ill with Covid-19 at a nursing home in the Swedish town of Märsta, a doctor consulted by phone ordered palliative care, including morphine, instead of trying to help him fend off the infection. Mr. Andersson’s son, Thomas Andersson, says he was told his father was too frail for other treatment. The younger man disagreed and, after arguing with the physician, summoned journalists and insisted his father be given lifesaving care. Mr. Andersson has since recovered.” [4]
In the same article in the WSJ is a graph showing the comparison of Swedish death rates to those of the other so-called Nordic wonders” (Figure 1).
It is already clear that Sweden’s death tally is one of the worst in the world’s developed countries (Figure 2):

Time magazine shows data from a study in JAMA comparing world-wide death rates, and strongly convinces that the USA and Sweden share a common pattern – of neglecting to react adequately to bring down high death rates (Figure 3):

But Figures 1 to 3 show crude death rates – even if adjusted for the population numbers in the countries. This practice was more or less standard. But significant problems concern how to accurately assign the ’cause of death’ – especially to COVID which has many ways of wreaking death. This has led many epidemiologists to call for more precise terminology. We will return to these authors later, but for example here is the view of some Swedish based epidemiologists:
“According to a recent report by WHO, Sweden is sharing the 12th place with the US on the list of countries with most COVID-19 deaths per million inhabitants. However, absolute death counts can be misleading and age- and sex-specific death rates should be used when comparing countries in order to account for differences in underlying age structure of both cases and the total population.COVID-19 death counts are inherently uncertain and inappropriate to compare between countries because they depend on the testing strategy in the population, on the principles for assigning cause of death, on whether only hospitalized deaths are considered or all deaths, etc.” [5]
In any case, the overtly obvious rising death rate in Sweden is becoming (or actually has become) a burgeoning kerfuffle in the Swedish population. The public are increasingly alarmed about this ‘non-aggressive’ behaviour of clinicians. I realise many leftists disdain ‘Time Magazine’ – but it has been perceptive on this matter. While it was not acceptable for many liberals and those on the Left to accept Boris Johnson’s government proclamations, or Trump’s government to imply that old people were dispensable – apparently it was OK for Swedish leaders to say this:
“From early on, the Swedish government seemed to treat it as a foregone conclusion that many people would die. The country’s Prime Minister Stefan Löfven told the Swedish newspaper Dagens Nyheter on April 3, “We will have to count the dead in thousands. It is just as well that we prepare for it.” In July, as the death count reached 5,500, Löfven said that the “strategy is right, I am completely convinced of that.” [6]
As Der Spiegel asks: “Hat Schweden die Alten geopfert? Has Sweden sacrificed the old?” – and answers ‘yes’. [7]
(2) The Concept of Excess Mortality – and what it shows in Sweden
Some epidemiologists do appear to be trying to minimise the death rates from COVID in countries such as Sweden. One particularly famous example of such an individual Prof. is John Ioannidis, based in Stanford and Berlin. He presents data for a statistic called “relative risk” of death. This – as its name implies shows the comparison of a rate as a function relative to another. Thus in Figure 4 the relative death rates of people over 65 are compared to those of people under 65 in various countries. This certainly shows that the rates of death are much higher in the elderly (by now not very much of a surprise), including in Sweden (Figure 4):
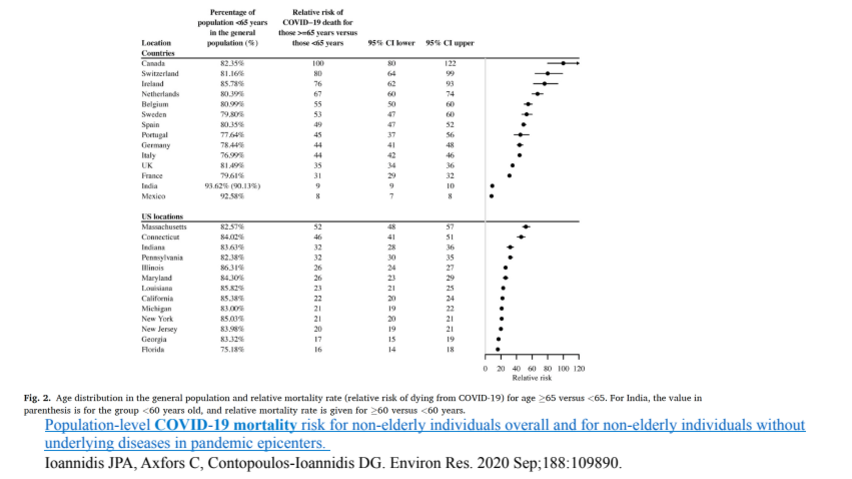
However the conclusions that Ioannidis et al draws are that:
“People <65 years old have very small risks of COVID-19 death even in pandemic epicenters and deaths for people <65 years without underlying predisposing conditions are remarkably uncommon. Strategies focusing specifically on protecting high-risk elderly individuals should be considered in managing the pandemic.” [8]
I believe this under-estimates the rates for younger people.
Here for example is a more specific age-categorised death rate for Sweden, showing values plotted against the median values of the prior years, averaged between 2015-2019 (Figure 5):

Again it can be seen that there is a higher mortality rate for the older sections of the population. But – it is also seen in the years above the age of 50 years. The rates in Figure 5 are described as ‘excess mortality’ but are categorised by age and sex-specific rates – rather than absolute rates.
Excess mortality is defined by other authors as:
“The gap between the deaths from any cause and the historical average for the same place and time of year, (which) offers a more comprehensive way to measure the mortality linked to the COVID-19 outbreak”.
These authors also describe a clear excess mortality for all causes of death across age groups in the Stockholm area (Figure 6) which clearly fall disproportionately on the low income group. [9] Figure 6:

3) Do masks and social distancing work to reduce rates of mortality?
We have written about the clear link between COVID deniers and open fascists, such as those in Germany of the AfD before (see Footnote 2). But we did not think in that article it was necessary to drill down into high-level evidence. However, as some ‘leftists’ are again disputing the evidence – here is some evidence as opposed to opinion.
Firstly there is a clear relationship between the wearing of masks and reducing death rates in countries with available data. Figure 7 below shows this clearly:

In words the authors express it in other ways – with a P value (this statistic tests how likely it is that the results of a study arise just by chance, the smaller the p value is the increasingly likely it is that the findings are ‘true’ and do not simply arise ‘by chance’ alone. A p value of less than (<) 0.05 is usually a criterion of approximating to ‘truth’):
“In a multivariable analysis of 196 countries, the duration of the outbreak in the country, and the proportion of the population aged 60 years or older were positively associated with per-capita mortality, whereas duration of mask-wearing by the public was negatively associated with mortality (all P < 0.001).” [10]
Finally, when social distancing policies are graded into a scale, there is a statistically significant relationship between both the incidence of COVID and the mortality from it. This means that social distancing reduces both rates of infection and death from COVID. This study was done in the USA, but although it has an NIH approval, it is not yet peer-reviewed. However, it appears that the more socially distanced policies result in lower death. [11] This is expressed in Figure 8 below:

Footnotes
Any attempt to downplay the effects of Swedish health policy in dealing with COVID – or should we say the failure of Swedish health policy – and a relationship to higher infection rates or death rates- is a white-wash.
1 How Should Marxists View the COVID-19 Pandemic of 2019-2020? March 17 2020
2 Looking Under the Hood – The Instrumentation of a Pandemic; November 30, 2020
3 Rafaela Lindeberg, Man Behind Sweden’s Controversial Virus Strategy Admits Mistakes; Bloomberg; June 3, 2020,
4 Bojan Pancevski, ‘Coronavirus Is Taking a High Toll on Sweden’s Elderly. Families Blame the Government. Discontent is growing over official triage guidelines critics say too often deny elderly patients vital care”; June 18, 2020; for The Wall Street Journal
5 Modig K, Ahlbom A, Ebeling M Excess mortality from covid-19. Weekly excess death rates by age and sex for Sweden and its most affected region. Eur J Public Health. 2020 Nov 10:ckaa218. doi: 10.1093/eurpub/ckaa218. Online ahead of print. PMID: 33169145
6 Kelly Bjorklund & Andrew Ewing The Swedish COVID-19 Response Is a Disaster. It Shouldn’t Be a Model for the Rest of the World’; Time Magazine, October 14, 2020.
7 Dietmar Pieper Berichte von Angehörigen und Recherchen zeigen, dass viele Covid-19-Opfer in Schweden noch leben könnten. “Man hat nicht versucht, ihr Leben zu retten”, sagt ein Virologe. 09.10.2020).
8 Ioannidis JPA, Axfors C, Contopoulos-Ioannidis DG Population-level COVID-19 mortality risk for non-elderly individuals overall and for non-elderly individuals without underlying diseases in pandemic epicenters. Environ Res. 2020 Sep;188:109890.
9 Calderón-Larrañaga A, Vetrano DL, Rizzuto D, Bellander T, Fratiglioni L, Dekhtyar S.
‘High excess mortality in areas with young and socially vulnerable populations during the COVID-19 outbreak in Stockholm Region, Sweden.’ BMJ Glob Health. 2020 Oct;5(10):e003595.
10 Christopher T. Leffler, Edsel Ing, Joseph D. Lykins, Matthew C. Hogan, Craig A. McKeown, and Andrzej GrzybowskiAssociation of Country-wide Coronavirus Mortality with Demographics, Testing, Lockdowns, and Public Wearing of Masks Am J Trop Med Hyg. 2020 Dec; 103(6): 2400–2411. PMCID: PMC7695060
11 VoPham T, Weaver MD, Hart JE, Ton M, White E, Newcomb PA Effect of social distancing on COVID-19 incidence and mortality in the US medRxiv. 2020 Jun 12:2020.06.10.20127589. doi: 10.1101/2020.06.10.20127589. Preprint. PMID: 32587998